It’s great to know that what a doctor can hear/feel in the physical exam of a patient with advanced heart failure is the best predictor of how well that patient will fare.
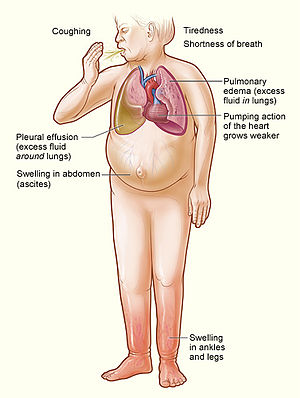
Despite the development of continually more sophisticated diagnostic tools, it’s comforting to know that the best guide to a patient’s prognosis is the doctor’s careful listening to and observation of four important indicators: 1) distended jugular venous distention, 2) a third heart sound, 3) rales (crackles) in the lungs, and 4) peripheral edema (swelling in the legs and ankles).
I am grateful that most doctors have some training in how to present bad news to a patient. As one of their duties, that’s gotta suck. But the hope is that patient and doctor have developed a respectful, caring relationship along the way.
Related articles